Understanding LLP Hair Loss: Causes, Symptoms, and Treatment Options
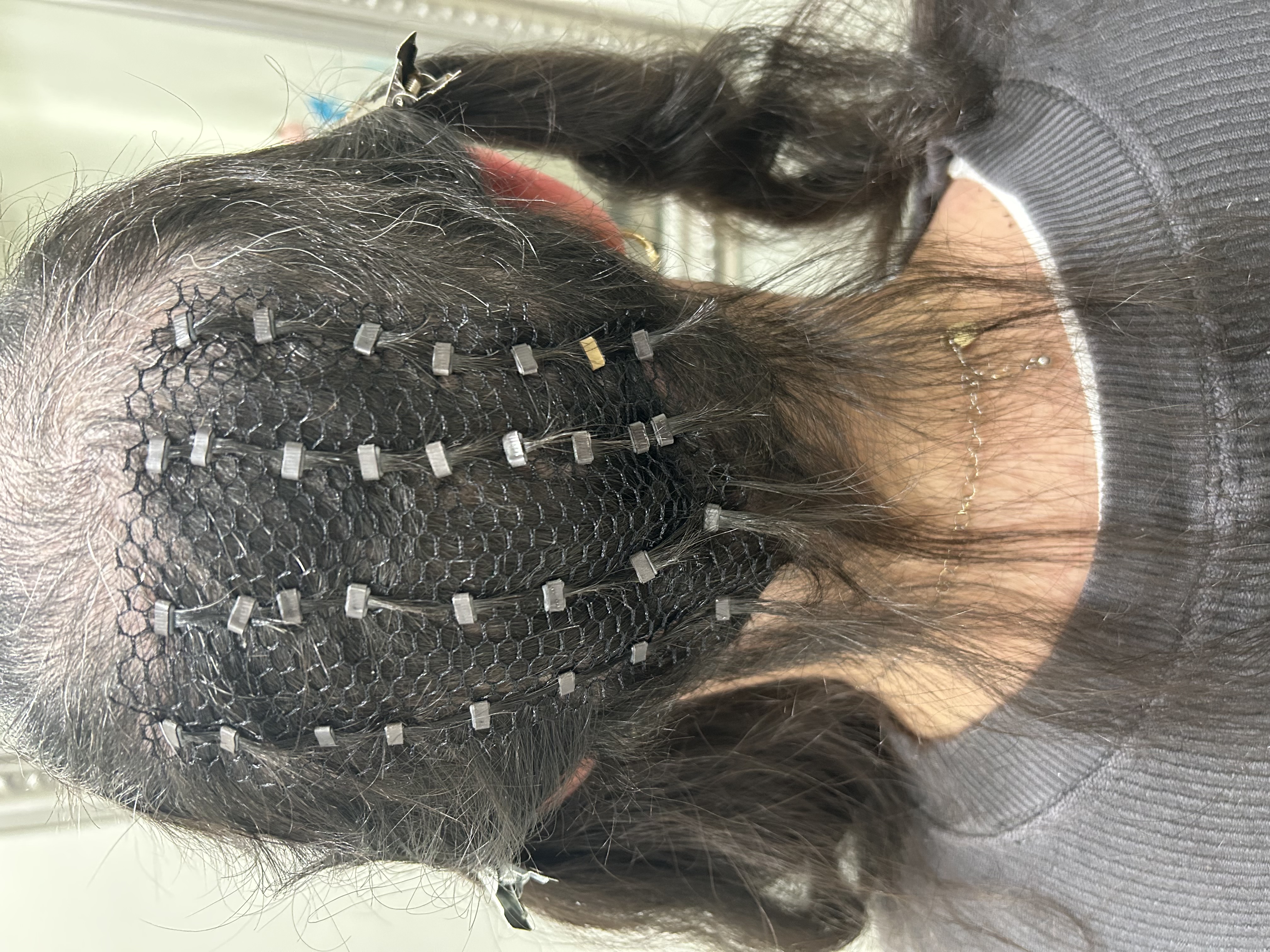
Lichen planopilaris (LLP) is a rare, inflammatory disorder of the scalp that attacks hair follicles and can lead to scarring alopecia. Because the damage can be permanent, understanding what LLP is, how it presents, and what can be done to slow or halt its progression is essential for anyone facing sudden thinning or patchy hair loss. This guide explains what drives LLP, who may be more likely to develop it, how dermatologists diagnose it, and the full range of treatments—from medications to daily care strategies—that can help protect your scalp and hair. We also explore practical ways to live well with this chronic condition, why early intervention matters, and how thoughtful styling choices can support both comfort and confidence. As you read, ask yourself: Are you noticing scalp symptoms you’ve been ignoring, and what small step could you take today to get clarity and support?
What is Lichen Planopilaris (LLP)?
Lichen planopilaris is a scarring form of hair loss caused by an immune response that targets the hair follicle. Without timely care, the inflammation can destroy follicles and prevent regrowth, leading to smooth, scarred areas where new hairs no longer emerge. Dermatologists typically confirm LLP with a clinical evaluation, trichoscopy, and in many cases a small scalp biopsy. Treatment aims to calm inflammation, ease symptoms like itching or burning, and preserve as many follicles as possible. Are you experiencing persistent scalp irritation or patchy shedding that hasn’t responded to routine haircare?
LLP is considered a follicular variant of lichen planus that primarily affects the scalp. In this autoimmune process, the body’s defenses mistakenly attack follicular structures, resulting in redness, tenderness, scaling, and progressive hair loss. Some find the disease flares in cycles, with calm periods followed by renewed activity. While there is no single test that captures the full picture, recognizing typical signs early and seeking specialty care can slow progression. Understanding the condition’s patterns and triggers places you in a stronger position to make informed choices. How might your daily routine change if you learned what sparks your own scalp flare-ups?
Though rare, LLP affects both men and women and is seen most often in adults, especially middle-aged individuals. The precise rate in the general population is low—well under 1%—yet the effect on quality of life can be significant due to visible hair loss, scalp discomfort, and the uncertainty of disease activity. Clinicians often begin treatment with topical corticosteroids to reduce inflammation and symptoms like itching. Would early attention to subtle signs—like increased shedding, scalp soreness, or scale—help you feel more in control?
The exact cause of LLP remains unclear, but the immune system clearly plays a central role. Genetic predisposition, hormonal shifts, infections, and stress may all act as contributors or triggers in susceptible people. Those with a personal or family history of autoimmune disorders may face higher risk. Although the science continues to evolve, learning how these factors interact helps guide long-term management. If you notice that periods of high stress worsen your scalp symptoms, could stress-reduction techniques be part of your plan?
Who Gets Lichen Planopilaris?
LLP can occur in adults of any gender but is diagnosed more frequently in middle-aged women. Individuals with lichen planus affecting the skin or mucous membranes may also be more likely to develop the scalp form. A background of autoimmune conditions in oneself or close relatives can raise the likelihood of LLP. Even with these patterns, anyone with persistent scalp symptoms should be evaluated early, since prompt care can preserve hair and improve comfort. Do you have a personal or family history of autoimmune conditions, and have you mentioned this to your dermatologist?
Although LLP is uncommon overall, its association with autoimmunity underscores the value of a thorough medical history. The timeline of hair changes, how quickly patches appeared, and where symptoms are most active all help clinicians tailor testing and treatment. The earlier inflammation is identified and addressed, the more likely it is to protect vulnerable follicles. If you could prevent further loss by seeking help sooner, what appointment would you schedule this week?
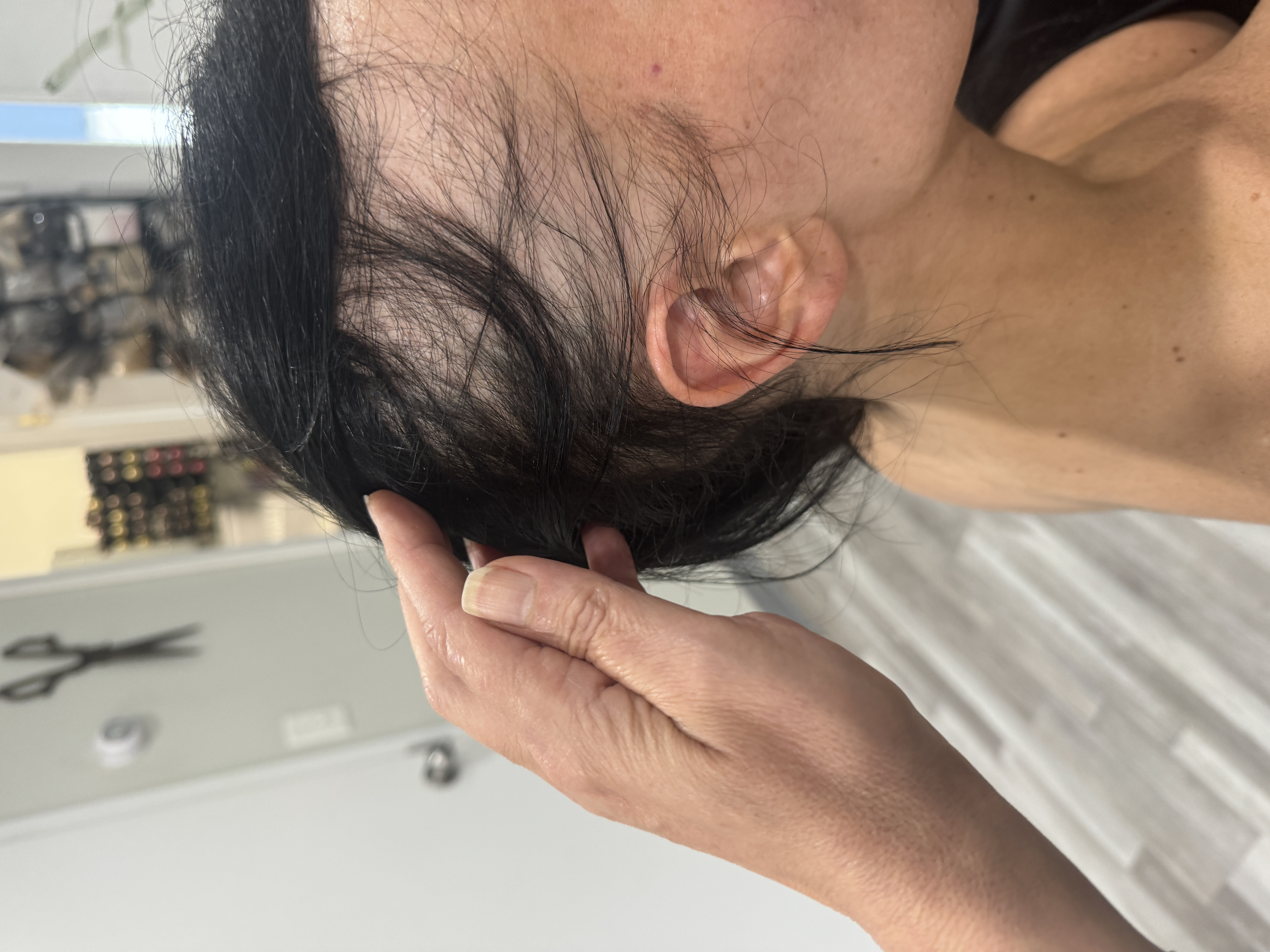
Causes and Triggers of LLP Hair Loss
LLP arises from an autoimmune attack targeting hair follicles. While genetic factors may contribute to susceptibility, the condition does not typically run strongly in families. Environmental and bodily triggers—including certain medications, infections, or hormonal fluctuations—may precede onset or intensify existing disease. The goal in clinical care is twofold: calm the immune reaction and reduce or remove triggers where possible. Have you noticed whether specific life events or new products preceded your scalp symptoms?
Because the condition can wax and wane, tracking flares empowers you and your care team to identify meaningful patterns. Keeping a simple journal that notes symptoms, stress levels, hair products used, and significant lifestyle changes can reveal insights over time. By recognizing your own triggers, you can refine your personal plan—one that protects comfort and supports long-term scalp health. What small tracking habit could you start today to better understand your scalp?
Stress, Hormones, and Flare-Ups
Stress and emotional upheaval have been linked to flares in many inflammatory conditions, and LLP is no exception. Major life changes, sleep disruption, and ongoing stressors may heighten symptoms like itching, tenderness, or new patches of hair loss. Hormonal changes—such as those around menopause—can also coincide with symptom shifts. Some patients report that infections or new medications preceded an LLP diagnosis. Identifying and minimizing personal triggers can reduce flare intensity, complementing medical treatment. When stress spikes, do you notice more irritation, sensitivity, or increased shedding?
LLP’s hallmark features include scalp discomfort, redness, scaling, and patchy hair loss that can become smooth and scarred if unchecked. Because early changes may seem like ordinary irritation or dandruff, subtle signs are often overlooked until patches enlarge. Timely assessment matters: once scarring is established, regrowth is limited. If you spot increased sensitivity or visible redness around follicles, how quickly could you consult a dermatologist?
Symptoms Checklist: Could It Be Lichen Planopilaris?
- Persistent scalp itching, burning, or tenderness that does not improve with routine haircare
- Redness around hair follicles or perifollicular scaling
- Patches of thinning or smooth hair loss without visible follicle openings
- Scalp discomfort that worsens during stressful periods or hormonal changes
- Areas of hair breakage near inflamed follicles
- Occasional shiny or white-appearing patches of scalp
- Sensitivity to tight hairstyles, harsh products, or heat styling
If several of these apply to you, a dermatology evaluation is recommended. Do these points sound familiar, and would documenting your symptoms help you prepare for an appointment?
Clinical Features and Diagnosis
In the early stages, LLP may present with redness, scale, and focal areas of thinning. Over time, patches can merge, leading to more extensive involvement and scarring. While LLP most commonly affects the scalp, in some cases features of lichen planus may be seen on the skin or mucous membranes elsewhere. Recognizing these patterns supports an accurate diagnosis and guides the choice of treatments that best match the disease’s activity level. Do you notice distinct “hot spots” on your scalp where symptoms cluster?
Diagnosis integrates a clinical exam, trichoscopy, and often a targeted scalp biopsy to evaluate inflammation around and within hair follicles. Trichoscopy can reveal absent follicular openings, perifollicular scale, and other characteristic patterns that help distinguish LLP from non-scarring hair loss. Additional testing—such as blood work—may be used to evaluate for other autoimmune processes. When results are combined, clinicians can distinguish LLP from similar conditions and start therapy promptly. Are you prepared to share a complete history of symptoms, medications, and styling routines at your visit?
Because LLP may resemble other types of alopecia, careful differential diagnosis is essential. It should be distinguished from frontal fibrosing alopecia and from non-scarring alopecia areata, which requires a different approach. Trichoscopy supports accurate separation from these conditions, and a biopsy can confirm when needed. A thorough exam of the skin, nails, and mucous membranes helps clinicians identify related signs consistent with lichen planus. Could seeking a second opinion from a scalp specialist offer additional clarity on your diagnosis?
Understanding LLP Across Different Skin Types
LLP’s fundamental process is similar across skin types, but how it appears can vary with pigmentation. In lighter skin tones, redness and white, smooth patches may be more visible, while in darker skin tones, affected areas may show darker pigmentation or post-inflammatory hyperpigmentation. Despite these appearance differences, the core symptoms—itching, sensitivity, scaling, and hair loss—remain similar. Has the visual presentation of your scalp symptoms made them easier or harder to recognize early?
Regardless of pigmentation, individualized evaluation ensures that color changes and texture differences are interpreted accurately. Early detection supports timely therapy, which is key to protecting hair follicles. If you have a darker skin tone, do you notice darker areas that persist after a flare has calmed?
Complications and Emotional Impact
Left unchecked, LLP can result in permanent hair loss in the affected areas. Some individuals may also notice thinning or loss of eyebrows or eyelashes, which can heighten self-consciousness. Beyond the physical findings, visible shedding and patchiness can cause significant emotional distress, including anxiety or low mood. A compassionate, comprehensive approach should address both medical care and emotional well-being. Would talking with a support group or counselor help you navigate the feelings that accompany hair changes?
An integrated plan may include medical therapy to slow the disease, mindful styling choices to reduce irritation, and cosmetic options to restore a sense of normalcy. Building a trusted care team—dermatologist, stylist, and supportive peers—can transform how manageable the journey feels. What one supportive resource could you add to your plan today?
Topical Steroids Only: Is That Enough?
Potent topical corticosteroids can be effective in mild or localized LLP by reducing inflammation and easing symptoms. Some individuals experience meaningful relief with topical therapy alone, especially when flares are limited. Others may require additional treatments when disease activity persists or spreads. Because response varies by person, ongoing monitoring helps determine whether a topical-only approach is sufficient. Have your symptoms calmed on topical therapy, or do you still notice new or enlarging patches?
Diagnosis and Differential Diagnosis of LLP
The diagnostic process typically includes a focused scalp exam, trichoscopy, and review of your medical and haircare history. If findings point to scarring alopecia, a small biopsy from an active area can clarify the type and severity of inflammation. This distinction matters because treatment strategies differ across scarring and non-scarring conditions. Are you documenting photos of your scalp to track changes over time?
Conditions that can mimic LLP include discoid lupus erythematosus and alopecia areata. Comprehensive history, targeted examination of nails and mucous membranes, and select lab tests help rule in or out these diagnoses. The sooner an accurate diagnosis is reached, the quicker an effective, personalized treatment plan can begin. Would a timeline of your symptoms and triggers help your provider pinpoint the most active areas to sample or treat?
Treatment Options for Lichen Planopilaris
LLP management targets inflammation, symptom relief, and follicle preservation. Therapies often start with potent topical corticosteroids to address active areas, sometimes paired with intralesional steroid injections for stubborn patches. If topical measures are insufficient or disease activity is widespread, oral agents—such as hydroxychloroquine or other immunomodulatory medications—and, in some cases, short courses of oral corticosteroids may be considered to calm the immune response. Treatments to support hair density, like topical minoxidil, can be layered with anti-inflammatory care when appropriate. Reported symptom-control rates vary by modality—for example, topical corticosteroids around 50–70%, intralesional treatments with similar rates for localized patches, and longer-term immunosuppressants often 60–75%—so tracking your response helps calibrate expectations. Which combination of treatments feels most aligned with your goals and comfort level?
Decisions are ideally customized based on how active the disease is, how quickly symptoms are changing, and which areas are affected. Collaboration with your dermatologist ensures adjustments can be made as your scalp responds. Understanding likely timelines, side effects, and relative success rates equips you to weigh options and participate confidently in shared decisions.
Common Pharmacological Treatments: Benefits and Considerations
- Topical corticosteroids (e.g., high-potency steroid solutions or foams): Often first-line for reducing redness, scale, and itch. Potential considerations include skin thinning or irritation with prolonged use; careful application under guidance helps lower risk. Typical symptom-control ranges are about 50–70%.
- Intralesional corticosteroids: Targeted injections into active patches can help slow inflammation locally. Temporary tenderness at injection sites may occur. Often similar success to topicals for localized lesions; risks include localized pain and temporary, mild skin atrophy.
- Hydroxychloroquine: An oral immunomodulatory option used to reduce autoimmune activity. Periodic monitoring is advised. Patients may notice gradual benefits over months.
- Calcineurin inhibitors (e.g., tacrolimus ointment): Non-steroidal topical agents that can ease inflammation, helpful for maintenance or in areas where steroid exposure needs limiting. Effectiveness can vary; some reports note about 50% symptom improvement.
- Systemic immunosuppressive agents (e.g., methotrexate or mycophenolate mofetil): Considered in refractory or more extensive cases to suppress persistent immune activity. These require medical supervision and routine labs. Long-term symptom control is commonly reported around 60–75%, with infection risk and liver-related effects requiring monitoring.
- Retinoids (e.g., acitretin): Sometimes used to influence the follicular environment and scaling; careful monitoring is essential.
- Topical minoxidil: Supports hair retention in non-scarred areas and can complement anti-inflammatory treatments. Scalp sensitivity should be monitored.
Every treatment choice involves balancing potential benefits against side effects, and response varies widely. Discuss your tolerance, preferences, and lifestyle with your dermatologist to build a plan you can maintain.
Non-Pharmacological Treatment Approaches
Supportive strategies can ease symptoms, help prevent further irritation, and complement medical therapy. While precise success rates are hard to quantify, many patients report fewer flares and improved comfort with steady routines:
- Dietary support: A balanced eating pattern rich in whole foods may support overall skin and immune health. Nutrients like omega-3 fatty acids and antioxidants are common in fish, nuts, seeds, fruits, and vegetables. Could a simple weekly meal prep help you maintain nourishing options?
- Stress management: Techniques such as mindfulness, breathwork, yoga, gentle movement, or journaling may help moderate flare frequency or intensity. What short daily practice could you adopt to lower stress load?
- Gentle scalp care: Use mild shampoos and conditioners and avoid harsh chemicals or excessive heat. Limit tight hairstyles that stress follicles. Incorporate brief, gentle scalp massage during cleansing to soothe and support circulation.
- Sun and heat protection: Hats and careful sun protection may reduce irritation on sensitive areas. Could a lightweight, breathable hat become part of your routine on bright days?
- Lifestyle tracking: Note flares alongside sleep patterns, major stressors, and product changes to spot patterns. Would a weekly photo log of your scalp help you notice subtle shifts earlier?
These steps are not substitutes for medical treatment but can significantly improve comfort and resilience.
Protective Styling, Wigs, and Hair Systems with LLP
Shielding the scalp from sun exposure with hats or sunscreen and avoiding harsh styling practices can reduce irritation. Gentle cleansing routines support scalp health. If patchiness is distressing, wigs and hairpieces can provide flexible coverage while medical treatment continues. Could a breathable, lightweight option help you feel more comfortable on high-symptom days?
From experience working with many people who have LLP, a clip-on hair system often suits sensitive scalps better than an attached topper. Attaching systems to inflamed skin can be uncomfortable and may complicate scalp care. Because LLP-prone scalps can become crusty or tender, access for cleansing and gentle massage is important. Wigs that are too heavy may feel hot or irritating. As a result, a clip-on option can strike a helpful balance between coverage and comfort. Have you tried different cap constructions to see which feels best during flare-ups?
When hair loss is under control, aesthetic solutions can complement medical care without blocking access to the scalp. At Noelle Salon, experienced hair-loss stylists can guide you through breathable designs and application techniques that respect ongoing treatment. If you are losing hair in specific zones, we may recommend carefully placed hair extensions that allow you or your clinician to continue topical therapy. Avoid applying soothing creams directly on attachment points to prevent slippage or buildup. Are you clear on which products are safe to use near extensions or clips?
Living with LLP: Building Daily Habits That Help
LLP is a chronic condition that often benefits from long-term, steady management. Regular follow-ups with your dermatologist help track whether the disease is active or quieting. Many people find it helpful to join support communities to share strategies, compare experiences, and build confidence through the ups and downs. Sticking with your agreed treatment plan and keeping the scalp clean and calm can make day-to-day life more comfortable. When setbacks occur, compassionate self-care and timely adjustments make a difference. What routine—weekly scalp checks, product reviews, or meditation—could anchor your self-care?
We approach LLP with care and practicality: soothing scalp treatments and gentle massage can be integrated before applying hair toppers or wigs, always prioritizing access for medical treatment. A private consultation offers a safe space to discuss symptoms, styling goals, and comfort concerns. As a rule of thumb, we discourage gluing systems onto the scalp during active loss or irritation. Would a trial fitting help you test comfort before committing to a particular system?

Clinical Course: What to Expect Over Time
LLP often follows a relapsing-remitting pattern, with active phases of inflammation and calmer intervals. Patients may present with smooth, white patches of hair loss where follicular openings are absent; redness and scale can border these areas. Symptoms such as itch, burning, or tenderness may signal ongoing activity. Without intervention, small patches can merge into larger areas. Trichoscopy helps identify absent follicles and perifollicular changes, while biopsy confirms the diagnosis when needed. Are you learning to recognize the earliest signs of a flare so you can start treatment quickly?
Because visible hair loss can carry a psychological burden, timely medical care and supportive styling can alleviate stress while the treatment plan takes effect. If a patch becomes smooth and scarred, regrowth is limited; the priority then is to contain further spread and optimize hair density elsewhere. Could planning for both medical and cosmetic steps in tandem help you feel more in control?
Key Terms: Simple Definitions to Reduce Confusion
- Scarring alopecia: Hair loss where follicles are permanently destroyed and replaced with scar-like tissue, limiting regrowth.
- Trichoscopy: Dermatoscopic examination of the scalp and hair follicles to identify characteristic patterns of disease.
- Perifollicular scale: Fine scaling around hair follicles, often seen in inflammatory scalp conditions.
- Autoimmune: When the immune system mistakenly attacks the body’s own tissues, such as hair follicles in LLP.
- Intralesional injection: A small amount of medication injected directly into active areas of disease on the scalp.
Having plain-language definitions can make appointments less stressful and decisions easier. Which term did you want clarified before your next visit?
Hypothetical Scenarios: Planning for Real Life
Scenario 1: The Sudden Flare — You notice a tender, itchy patch that seems to grow over several weeks. You schedule a dermatology visit, start a topical steroid, and use a mild, fragrance-free shampoo. You also pause tight hairstyles and add a breathable hat for sun protection. Your symptoms begin to calm, and you track progress with weekly photos. Would creating a short, written “flare plan” help you act faster next time?
Scenario 2: Styling with Sensitivity — You have several small, stable patches. You choose a lightweight, clip-on topper for coverage and plan regular removal for gentle cleansing and scalp checks. During high-symptom days, you swap to a soft scarf or a cap. Because you avoid adhesives during flares, your scalp remains more comfortable. What styling adjustment could make the biggest difference in your comfort?
Scenario 3: Long-Term Stability — Your disease becomes quieter with a steady routine: maintenance topicals, consistent stress reduction, and periodic follow-ups. You keep products simple and avoid harsh treatments. With this foundation, your confidence grows, and you feel prepared to handle a flare if one appears. Could building a small, reliable routine be your path to steadier days?
Prognosis and Long-Term Outlook
Outcomes vary with LLP. Some individuals experience periods of stability or gradual improvement, while others face persistent activity that requires ongoing therapy. Early, consistent care can make a major difference in preserving hair and minimizing symptoms. Long-term effects may include areas of permanent loss and the emotional impact of visible thinning. Yet with patient, steady management, many people find an approach that reduces flares and supports daily comfort. What proactive step—booking a consult, simplifying products, or starting a stress practice—could you take today to support your future self?
Adherence to your plan, openness about side effects, and timely adjustments help maintain momentum. Because LLP is unpredictable, regular check-ins allow you and your provider to respond quickly to changes, protecting scalp health over time. Are you ready to create a follow-up schedule that keeps you on track without feeling overwhelming?
Guided Cosmetic and Aesthetic Support
When medical treatment has reduced active inflammation, aesthetic solutions can restore confidence without disrupting scalp access. Strategically placed hair extensions may be used away from sensitive areas, and lightweight toppers can blend seamlessly with your natural hair. Avoid placing soothing creams on extension attachment sites to maintain hold and cleanliness. Have you considered a consultation to explore options that respect your scalp’s changing needs?
We recommend clip-on systems when the scalp is irritated and strongly discourage gluing hair systems during active loss. Treatments like gentle massage can help comfort the scalp prior to applying toppers or wigs. With thoughtful styling, you can maintain access for medications and cleansing, keeping both aesthetics and scalp health in balance. Do you have a go-to look that feels both comfortable and confidence-boosting?
Practical Do’s and Don’ts for LLP Hair Loss
- Do prioritize early evaluation for persistent itching, burning, or patchy loss.
- Do use gentle haircare products and minimize heat or chemical exposure.
- Do protect your scalp from intense sun and reduce friction from tight styles.
- Do track symptoms and triggers to guide care decisions.
- Don’t apply adhesives or harsh treatments to inflamed or crusted areas.
- Don’t ignore new tenderness or rapid shedding—seek prompt advice.
- Don’t stop medications suddenly without discussing with your dermatologist.
Small, consistent choices add up over time. Which one “Do” will you commit to this month?
Reader Challenge: Share Your Strategies
Living with LLP is a journey best traveled with support. In the comments, consider sharing the routines, products, or mindset shifts that brought you the most relief. Your experience may help someone else take their next step with more confidence. What tip or encouraging word would you offer to someone newly diagnosed?
Conclusion: Take Charge of LLP Hair Loss
Lichen planopilaris is a scarring hair loss condition driven by immune-related inflammation of the hair follicles. While it is rare, its impact on daily life and self-image can be profound. Early diagnosis, tailored medical treatment, and thoughtful daily care can limit progression and improve comfort. Pharmacological options—from topical steroids to systemic immunomodulators—aim to quiet inflammation, while supportive strategies like gentle scalp care, stress reduction, and sun protection help prevent irritation. Cosmetic solutions such as lightweight wigs, toppers, or carefully placed extensions can restore a sense of normalcy without disrupting access for treatment.
Define your next action: schedule a dermatology appointment, simplify your haircare routine, or explore comfortable coverage options that honor your scalp’s needs. With knowledge, a supportive team, and a steady plan, you can navigate LLP with greater clarity and control. Which step will you take today to protect your scalp and strengthen your confidence?




