Understanding and Managing Trichotillomania (Hair Pulling Disorder) and Crinkly Hair Strands: Essential Strategies
-
Learn the basics and personalize your plan: spend 10 minutes reviewing core facts about trichotillomania, then write down 2–3 ways it affects your mood, self-esteem, and daily life.
-
Book professional support: schedule an assessment with a qualified clinician, ask about CBT and habit reversal training, discuss whether medications like SSRIs are appropriate, and set one clear first goal.
-
Identify your triggers: keep a daily journal noting time, place, activity, emotions, and sensations before/after pulling; review it weekly to spot patterns that lead to urges.
-
Build alternatives and barriers: assemble a hand-busy toolkit (stress ball, fidget items, textured fabric), choose a competing response to practice during urges, and use stimulus control (e.g., store tweezers out of reach, wear finger covers during high-risk times).
-
Enlist a support system: tell 1–2 trusted people about your goals, schedule regular check-ins, and agree on how they can help (distractions, reminders, or encouragement during tough moments).
-
Reinforce progress and refine: set small rewards for milestones, practice 5–10 minutes of mindfulness or breathing daily, and adjust your plan weekly using your notes or clinician feedback.

Introduction to Trichotillomania and Hair Pulling
Trichotillomania, often called hair-pulling disorder, is a mental health condition in which a person experiences a persistent, hard-to-resist urge to pull out their own hair. In some cases, hair pulling is followed by trichophagia, where an individual may ingest the hair. While the behavior can bring momentary relief, the longer-term effects may include hair loss, scalp irritation or injury, and intense emotional distress. Many people describe the cycle as a brief calm or satisfaction during pulling, followed by guilt, shame, or worry about appearance and social reactions.
Managing trichotillomania usually involves a comprehensive plan that blends understanding the condition, identifying personal triggers, seeking professional guidance, and practicing practical coping skills. Treatment can include therapeutic approaches—especially cognitive behavioral therapy (CBT) and habit-focused interventions—as well as medications like selective serotonin reuptake inhibitors (SSRIs) when recommended by a clinician. Support from healthcare providers and loved ones helps individuals move toward more consistent symptom relief.
In this blog, we will explore the essentials of understanding trichotillomania, how to recognize its symptoms, what can contribute to hair-pulling urges, and actionable strategies for treatment and self-management. Whether you live with trichotillomania or support someone who does, the guidance below can help reduce hair pulling and improve daily life.
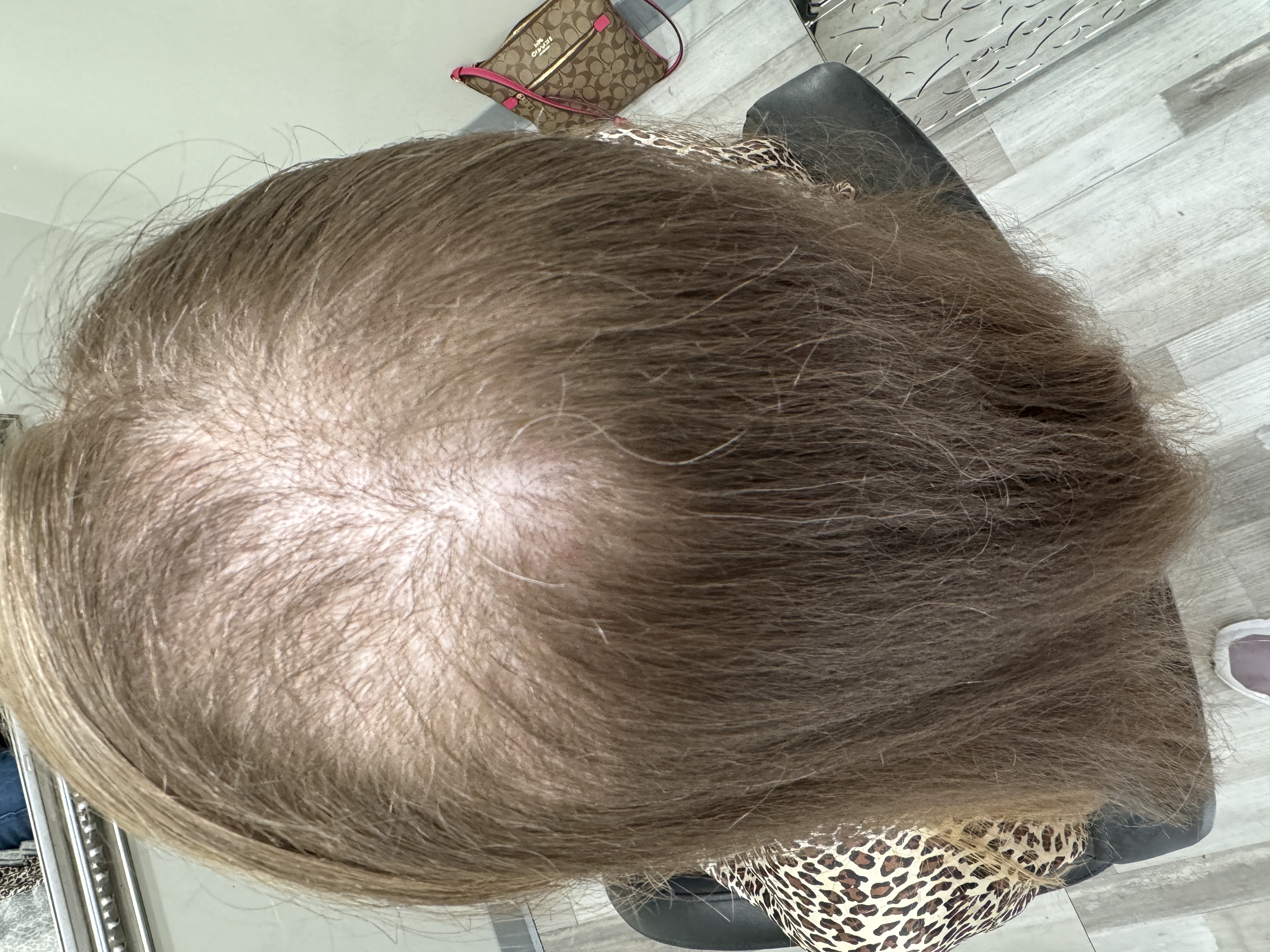
Understanding Trichotillomania: Hair Pulling and Its Impact
Trichotillomania is related to obsessive-compulsive and related disorders and is characterized by recurrent hair pulling that leads to noticeable hair loss. Urges and compulsions can start in childhood or adolescence and may persist into adulthood if left untreated. Emotional effects—such as shame, embarrassment, and lowered self-worth—often compound the challenge and can make it harder to reach out for help. With professional support and practical strategies, however, many people reduce pulling and experience meaningful improvements in daily functioning and mood.
Defining Trichotillomania (Hair Pulling Disorder) and Its Focus on Hair
Trichotillomania involves a powerful urge to pull hair from areas like the scalp, eyebrows, and eyelashes, as well as other body regions. The act of pulling can briefly relieve tension or provide gratification, which reinforces the habit and makes it more likely to recur. Over time, this cycle can create visible consequences and emotional strain.
The scalp is a common focus area, where repeated pulling may cause patchy hair loss, thinning, or breakage. Chronic pulling can irritate follicles, causing small bald patches or uneven density. Eyelashes and eyebrows can also be affected, leaving sparse or missing hairs that may alter appearance and confidence. Many individuals describe seeking out coarse or oddly textured hairs because finding and removing them initially creates a sense of relief or “rightness,” even though negative feelings often follow soon after.
The Psychological Impact of Trichotillomania and Hair Pulling
While hair pulling can soothe tension for a moment, it frequently brings up feelings of stigma, guilt, or embarrassment. The visibility of hair loss can lead to self-consciousness, avoidance of activities, and worries about how others might respond. Children and adolescents may struggle socially or at school, and adults might find relationships, work performance, or daily routines disrupted by urges and the time spent managing them.
Despite these challenges, change is possible. With the right tools and support, many people report fewer urges, longer pulling-free periods, and a stronger sense of control. Care from trained clinicians, along with self-help methods and compassionate support systems, can help rebuild confidence.

Trichotillomania Symptoms: Recognizing Hair Pulling Signs and Triggers
Trichotillomania typically includes:
- Recurrent pulling out of hair that leads to visible hair loss or breakage
- Repeated efforts to reduce or stop hair pulling with limited success
- Significant distress or disruption to social, school, or work life
- Time spent searching for certain hairs (e.g., coarse, wiry, or “kinky” strands) to pull
- Rituals around pulling (e.g., feeling the hair root, examining strands, or specific times/places where pulling occurs)
Recognizing these signs early helps guide next steps—such as tracking triggers, speaking with a clinician, and trying targeted coping skills to reduce the frequency and intensity of urges.
Recognizing Hair Pulling Signs in Yourself or Others
Common signs include thinning areas, uneven hair lengths, or bald patches on the scalp, as well as sparse eyelashes or eyebrows. You might notice hands frequently moving toward hair, feeling for irregular or kinky hairs, or twirling strands. Some people report a building sense of tension before pulling and a short-lived relief afterward, followed by disappointment or frustration.
If you suspect trichotillomania in yourself or a loved one, gentle conversation and practical support can make a difference. A dermatologist can assess hair and scalp concerns, while a mental health professional can evaluate symptoms, suggest treatment options, and collaborate on a plan to reduce pulling. Early support helps interrupt the cycle and promotes healthier coping.
The Specifics of Crinkly Hair Strands From Hair Pulling
Crinkly or irregular strands often result from repeated pulling and partial breakage along the hair shaft. These fractured hairs can feel rough or uneven to the touch. Because the texture stands out, it can draw more attention and trigger further pulling, especially when stress or strong emotions are present.
Although hair pulling can become an ingrained habit, it is changeable. Many people learn to interrupt the cycle with structured strategies, stress reduction, and practical environmental tweaks that make pulling less likely. Working with a clinician—and practicing alternative responses—helps reduce harm to hair and scalp while building a sense of control.

Causes Behind Trichotillomania and Hair Pulling Urges
The exact cause varies by person, with psychological, genetic, and environmental factors all playing a role. Some people pull in response to anxiety or strong emotions; others do so almost automatically during passive activities like reading or watching TV. Mapping your patterns helps tailor strategies that fit your life.
Common Environmental Triggers for Hair Pulling
Specific settings and sensory cues can nudge urges, especially when stress is high:
- Social anxiety: meetings, classes, or gatherings that raise self-consciousness
- Boredom or inactivity: waiting rooms, long commutes, or monotonous tasks
- Mirrors and reflective surfaces: appearance-checking or scrutinizing perceived “flaws”
- Easy access to tools: tweezers, magnifying mirrors, or hair accessories within reach
- Sensory cues: feeling a loose hair on the neck/scalp or certain fabric textures against skin
- Stressful events: deadlines, family conflict, or major life changes
Keeping a brief trigger log helps you spot these patterns and plan small environmental tweaks—like relocating tools or limiting mirror time—so urges are less likely to escalate.
Psychological and Genetic Factors in Trichotillomania
Psychological drivers—shame, guilt, tension, or a desire to “correct” an irregular hair—can intensify urges. Paired with the brief relief after pulling, they strengthen the habit loop. Learning to identify thoughts, feelings, and sensations that precede pulling is central to treatment.
Genetic factors may also increase susceptibility to compulsive behaviors. Concerns about appearance (e.g., body image or body dysmorphic symptoms) can fuel a cycle of focusing on perceived imperfections and trying to “fix” them by pulling. Addressing both emotional and behavioral components often produces the best outcomes.
Effective Treatment Strategies for Hair Pulling Disorder
Comprehensive treatment blends structured therapy with practical self-management tools. Many people benefit from cognitive behavioral approaches—especially habit reversal training—while others may add medications to address co-occurring symptoms or reduce the intensity of urges. The most effective plans are collaborative and personalized, with clear goals, regular check-ins, and flexible adjustments as needs change.
Behavioral Therapy Approaches to Reduce Hair Pulling: Professional Therapies for Trichotillomania
Cognitive behavioral therapy (CBT) is a leading approach for reducing hair pulling. It helps you identify triggers, challenge unhelpful thoughts, and practice new responses that interrupt the pulling cycle. A key CBT method is habit reversal training, which includes:
- Awareness training: learning to notice early signs of urges and the contexts in which pulling typically happens
- Competing response practice: substituting a specific action (e.g., clenching fists, squeezing a stress ball, or pressing palms together) until the urge passes
- Stimulus control: changing the environment to reduce triggers, such as wearing finger covers while reading or keeping hands engaged during passive activities
Some individuals also explore hypnotherapy as a complementary approach. By using guided relaxation and focused suggestion, sessions aim to help modify automatic responses linked to hair pulling. When combined with behavioral strategies, these techniques can support greater awareness and impulse control.
Medications for Trichotillomania and Hair Pulling Urges
Medications can be part of a broader plan. Tricyclic antidepressants like clomipramine and selective serotonin reuptake inhibitors (SSRIs) are sometimes used to help manage urges and co-occurring symptoms. Medication decisions should be made with a qualified clinician, who can monitor response and side effects and coordinate care with a therapist. Treatment plans often work best when medication and therapy are integrated and adjusted based on progress.
Also Read: Best Hair Growth Products for Trichotillomania
Self-Help Techniques for Managing Trichotillomania
Self-guided strategies complement professional care and help you practice skills daily. Consider a simple checklist you can reference quickly:
- Track patterns: note times, places, activities, thoughts, and sensations that precede pulling
- Prepare alternatives: keep tactile tools handy (stress balls, fidget rings, textured fabrics)
- Plan competing responses: decide in advance which action you’ll use when an urge arises
- Adjust environments: add gentle barriers (headbands, hats) or keep hands occupied during triggers like TV time
- Build routine breaks: schedule brief movement, stretching, or relaxation between tasks
- Reinforce wins: acknowledge small successes and practice self-compassion after slip-ups
Behavioral Modification to Reduce Hair Pulling
Behavior change works best when it is specific and repeatable. Try these steps:
- Habit reversal training: pair awareness of early cues with a planned competing response for 1–2 minutes
- Stimulus control: relocate tweezers or mirrors out of sight; wear gloves or bandages on fingers during high-risk times
- Urgency scaling: rate the intensity of an urge from 1–10 and delay pulling for a set interval while using a competing response
- Replacement behaviors: braid hair, wear a loose cap, or style hair in ways that limit access to targeted areas
- Reward consistency: track streaks and celebrate each step forward, even if progress is uneven
Stress Management and Relaxation Practices for Hair Pulling Triggers
Stress management reduces the emotional fuel behind urges. Start by identifying top stressors and experiment with practical resets—brief walks, deep breathing, stretching, or short meditations. Establish boundaries around work and rest, prioritize sleep, and build small routines that promote calm.
Relaxation techniques can be woven into daily life: mindfulness practices, soothing music, warm showers, gentle yoga, journaling, or crafting. The goal is to lower baseline tension so urges are less frequent and easier to navigate when they arise. Choose two to three techniques to practice consistently, and add more as they become habits.
Seeking Support for Hair Pulling Challenges: The Role of Support Systems
Reliable support eases isolation and keeps change on track. A strong network offers empathy, perspective, and accountability. For many, sharing progress and setbacks with trusted people helps reduce shame and makes it safer to ask for help when urges peak.
Seeking Support for Hair Pulling: Finding and Utilizing Support Groups
Support groups—online or in person—offer a place to connect with others who understand hair pulling. Group conversations can provide practical tips, encouragement, and a sense of community. Many groups also share educational materials, coping strategies, and professional insights that reinforce skills you’re building in therapy.
How Family and Friends Can Help with TTM Hair Pulling
Families and friends can create a compassionate environment by learning about trichotillomania, listening without judgment, and reinforcing healthy coping steps. Useful actions include:
- Asking how to help during tough moments and following the person’s lead
- Offering gentle distractions—short walks, games, or hands-on activities—when urges spike
- Celebrating small wins and progress, rather than focusing on slip-ups
- Encouraging professional support and helping with logistics (appointments, reminders)
Differential Diagnosis: Hair Loss Conditions vs. Hair Pulling Disorder (Trichotillomania)
Several conditions can resemble trichotillomania-related hair loss. A thorough clinical assessment—often including a scalp examination and, when indicated, a biopsy—helps clarify the cause:
- Trichotillomania: recurrent hair pulling with noticeable loss; pulling usually brings relief or gratification and is often linked to identifiable urges or routines
- Alopecia areata: patchy hair loss without pulling behaviors; autoimmune in nature
- Traction alopecia: thinning or loss due to sustained tension from certain hairstyles or extensions; behavioral pulling is not the driver
- Tinea capitis: fungal infection that can cause hair loss and is often associated with scalp scaling or redness
For example, a smooth, coin-sized bald patch that seems to appear overnight without any pulling points to alopecia areata. Thinning along the hairline or temples in someone who consistently wears tight ponytails or braids suggests traction alopecia. An itchy, scaly, red patch with tenderness indicates tinea capitis, whereas trichotillomania is more often marked by irregular broken hairs of different lengths, recognizable urges or routines to pull, and brief relief followed by frustration.
Recognizing these distinctions is important because the most effective treatment depends on the underlying cause. In trichotillomania, behavioral and supportive strategies are central; in other conditions, dermatologic treatments may be prioritized.
Conclusion: Living Well with Trichotillomania and Hair Pulling
Managing trichotillomania involves understanding how hair pulling operates, identifying personal triggers, and applying strategies that interrupt the cycle. Therapies like CBT and habit reversal training, possible medication support, and practical self-help techniques work best when paired with consistent stress reduction and a caring support system. Many people grow more confident, experience fewer urges, and protect hair and scalp health. Reaching out for help, learning about the condition, and building a supportive environment make progress more achievable, even when change feels slow.
Frequently Asked Questions About Trichotillomania and Hair Pulling
What Makes Crinkly Hair Strands More Prone to Pulling?
Crinkly hair strands can feel different—rougher or irregular—making them stand out when touched. The distinctive texture may capture attention and prompt pulling, especially in moments of stress or boredom. Preparing alternatives (like fidget tools) and practicing competing responses can reduce the urge to manipulate these strands.
Why do I have random strands of wiry hair?
Genetics and natural texture variations can create wiry strands, and texture can also change with age or hormonal shifts. If these stand-out hairs trigger pulling, try tactile substitutions and styling choices that reduce access. Embracing your unique texture while strengthening coping skills helps limit the cycle.
Can trichotillomania change hair texture?
Frequent pulling can damage hair follicles and break shafts, which may change how regrowth looks or feels in targeted areas. Reducing pulling through therapy and self-help strategies helps protect follicle health and supports more consistent regrowth over time.
What are common triggers for hair pulling?
Triggers vary, but certain patterns are frequent. Situational triggers can include stress, boredom or inactivity, emotional distress (like anxiety or frustration), and physical sensations such as noticing split ends or an uneven texture on the scalp.
- Stressful events: exams, deadlines, interviews
- Boredom: passive activities without hand engagement
- Strong emotions: anxiety, sadness, irritation
- Physical cues: feeling coarse or uneven strands
How can I identify my personal triggers?
Keep a brief journal of pulling episodes to spot patterns. Note the time, location, what you were doing, and your emotions or sensations right before the urge.
- Time of day
- Environment (home, work, public)
- Activity just before pulling
- Emotional state and physical sensations
What long-term strategies help manage trichotillomania?
Plan for maintenance, not perfection. Build steady routines that keep skills fresh and support in place.
- Regular therapy check-ins to adjust strategies
- Participation in support groups for accountability and encouragement
- Medication reviews if prescribed, with scheduled follow-ups
- Maintenance goals every few months to sustain motivation
How can I prevent relapse?
Create a simple relapse-prevention plan you can use quickly when urges rise. Keep it visible and share it with a trusted person.
- Revisit your journal to update known trigger patterns
- List go-to competing responses and alternative activities
- Alert your support system early for reminders and encouragement
Living With Trichotillomania: Day-to-Day Hair Pulling Management
Day-to-day life with trichotillomania involves managing both emotional and physical effects. Many people benefit from routines that balance self-care, workable coping skills, and supportive relationships. Consider a personalized plan that includes a short morning check-in (identify stressors and supports), planned breaks to manage tension, and an evening reflection to note wins and refine strategies. Open conversations about the condition can reduce isolation and help loved ones offer practical support.
Enhancing Healthcare Team Outcomes in Trichotillomania and Hair Pulling Care
Collaborative care brings together psychiatry, psychology, dermatology, and primary care to address therapy, medication, and skin/hair health in a unified plan.
- Mental health clinician/therapist: provides assessment, CBT, and habit reversal training; helps map triggers and build coping skills.
- Dermatologist: evaluates scalp and skin injuries, hair loss, and regrowth; offers guidance on protecting follicles and treating irritation.
- Prescribing clinician (psychiatrist or primary care): considers medications such as SSRIs, tracks benefits and side effects, and adjusts as needed.
- Collaborative care team: coordinates updates so therapy, medication, and physical care are aligned and mutually reinforcing.
Regular follow-ups and shared goals keep everyone aligned, while your notes about tough times or settings help the team fine-tune strategies that fit your life.




